Ileal Interposition and Hormonal Mechanisms of Action
Ileal Interposition surgery is a digestive system procedure which changes alignment of small intestines. Ileal Interposition causes very different metabolic changes with this new ordering in the digestive system. These metabolic changes created provide complete normalization of Metabolic Syndrome findings including diabetes. The actual cause underlying all these treatments is hormonal changes created by Ileal Interposition surgery.
Although Ileal Interposition surgery is a digestive system procedure applied on stomach and small intestines anatomically, it may be defined as endocrine surgery in terms of effects. Because it does not present its effects by reducing the absorption. All results appeared after Ileal Interposition appear by regulation of hormonal secretion to increase insulin effect and reduce insulin resistance.
Sleeve Gastrectomy
ILEAL TRANSPOSITION IN STAGES
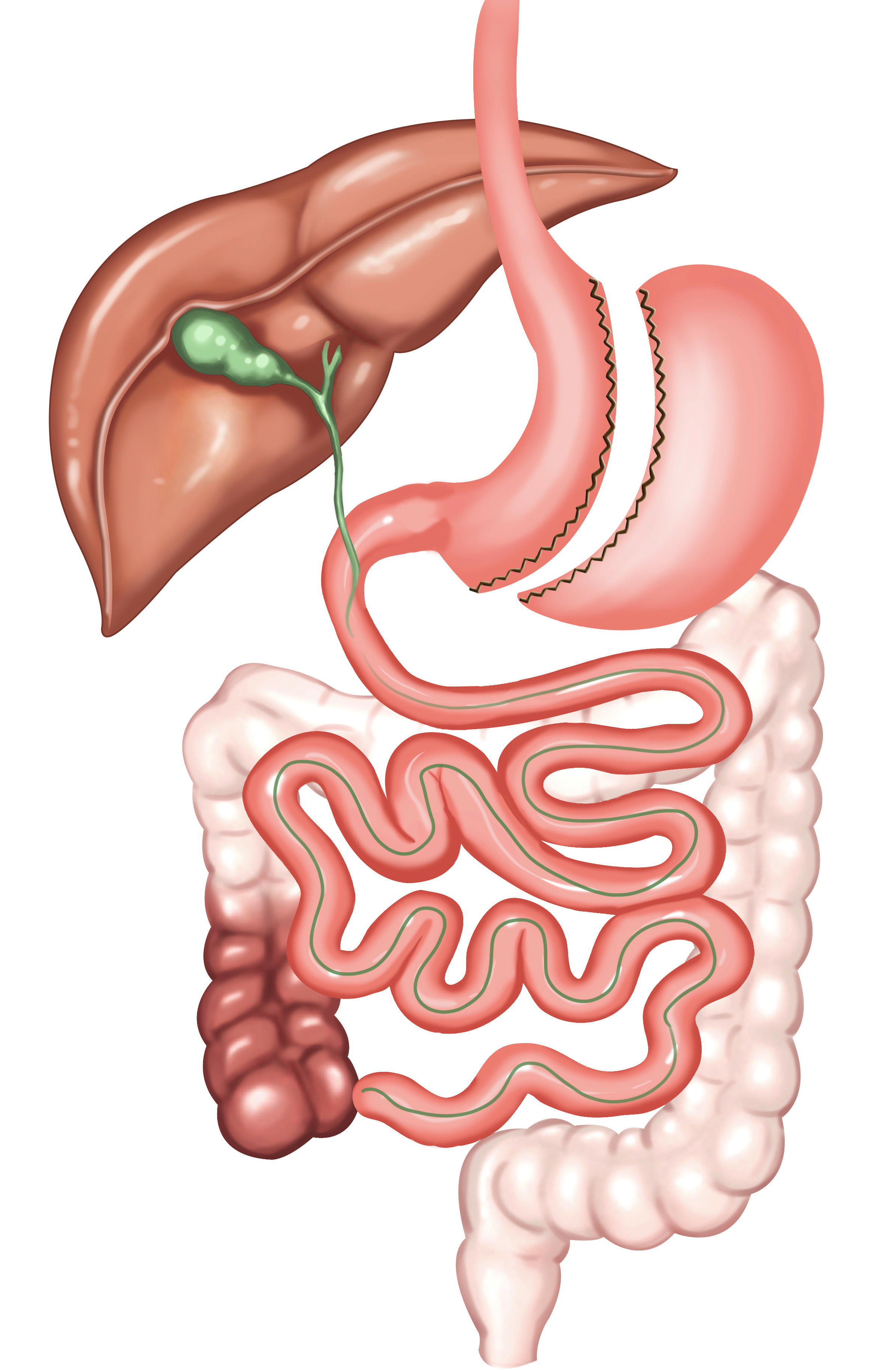 1. Sleeve Gastrectomy (Gastric Tubing)
1. Sleeve Gastrectomy (Gastric Tubing)
The first section of Ileal Interposition surgery is removal of the stomach longitudinally. This procedure is called Sleeve Gastrectomy (Gastric Tubing). Gastric tubing procedure applied in Ileal Interposition is same with gastric tube surgery applied for obesity surgery. The only and important difference is that Sleeve gastrectomy applied for Ileal Interposition leaves a wider gastric pouch for those applied for obesity.
The actual purpose for partial removal in Ileal Interposition surgery is to reduce hunger hormone called Ghrelin. Ghrelin plays a role in insulin resistance. By reduction of Ghrelin hormone, a factor suppressing hormonal effects of insulin and hunger sense is suppressed.
2. Duodenal Exclusion (Separation of Duedonum from Stomach)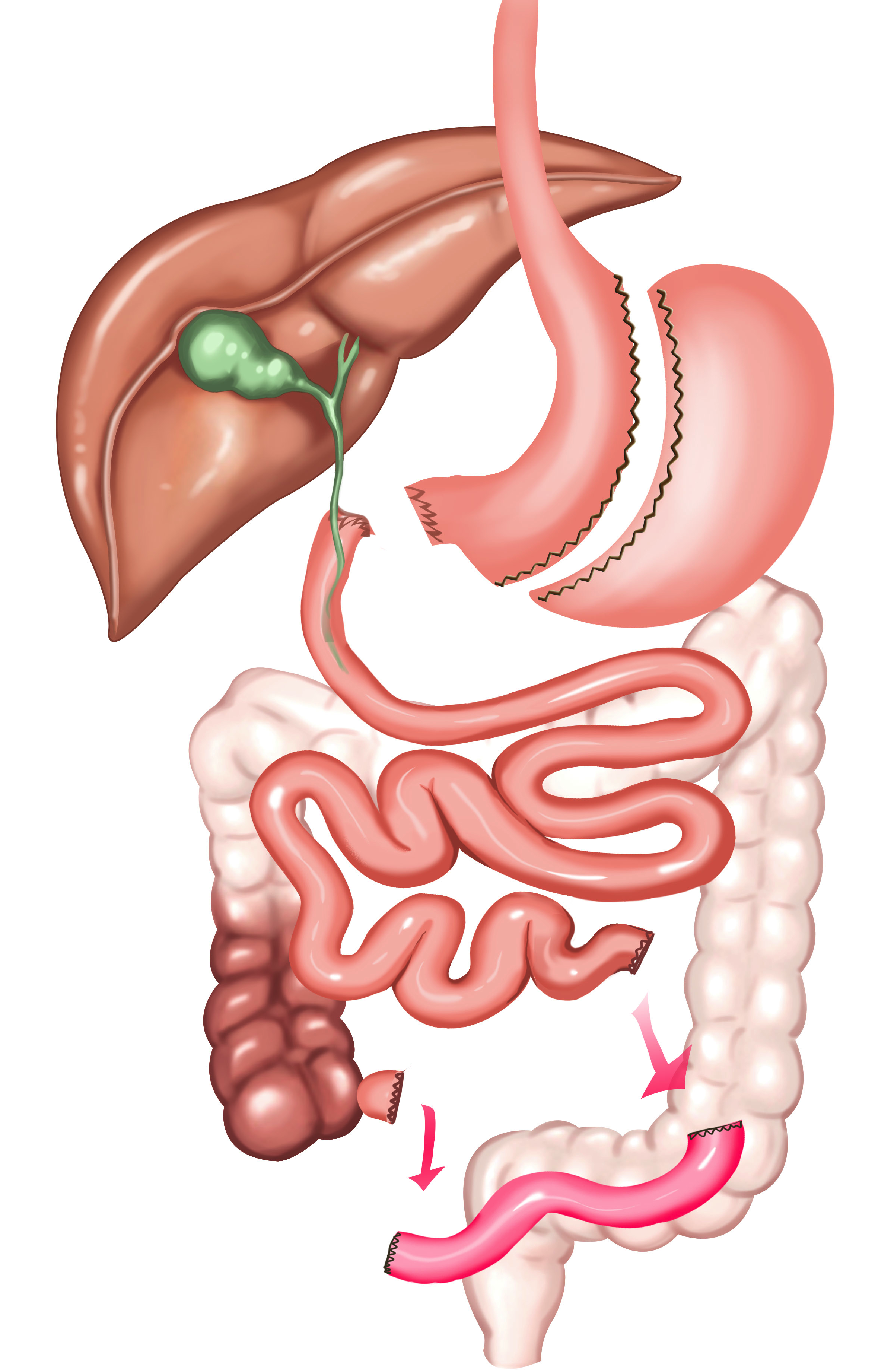
Duodenal Exclusion
Ileal Interposition surgery uses different mechanisms of action that metabolic surgery operates in different operations together.
Power of action of Ileal Interposition surgery becomes superior than all methods known.
The procedure called Duodenal Exclusion is one of the most important action mechanism of Ileal Interposition operation. Duedonum is separated from the stomach by Duodenal Exclusion. So, foods can not pass into duedonum. It is believed that separation of duedonum from foods provides reduction of secretion of anti-incretin factors which reduces effect of insulin hormone.
Furthermore, function of the hormone secreted from duedonum and called GIP (Glucose Induced Polypeptide – Gastrointestinal Polypeptide) is increased by this way. Serum quantity of GIP hormone does not decrease in diabetic patients but functionality is spoiled. Efficiency of GIP hormone increases in diabetic patients after duodenal exclusion procedure. So, activities, namely viability of insulin producing beta cells are supported.
3. Ileal Interposition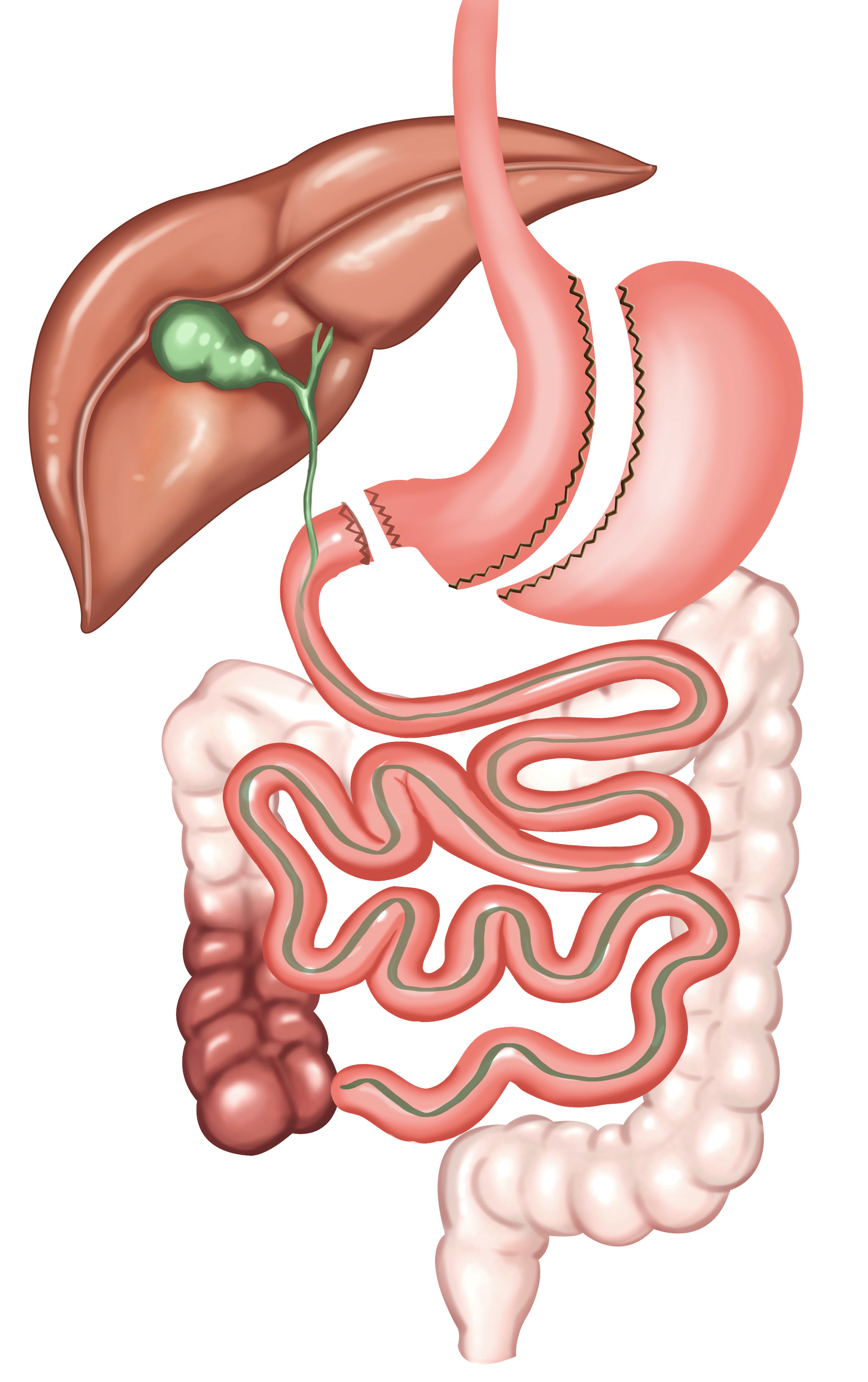
Preparation of Ileum Segment
Ileal Interposition means addition of “ileum” which is the last part of small intestine into the beginning part. We call this addition procedure as “interposition”. It means repositioning or interposition. The actual mechanism of action of the surgery is this interposition procedure. This procedure is performed within several stages.
i. Preparation of Ileal Segment
First, a piece from "ileum" which is the last psrt of smll intestine is separated. This separated part is called “ileal segment”. This ileal segment will be connected to gastric exit then.
ii. Ileo-Ileal Anastomosis
By removal of ileal segment, two intestinal ends which are liberated are combined. So, continuity of intestines are provided.
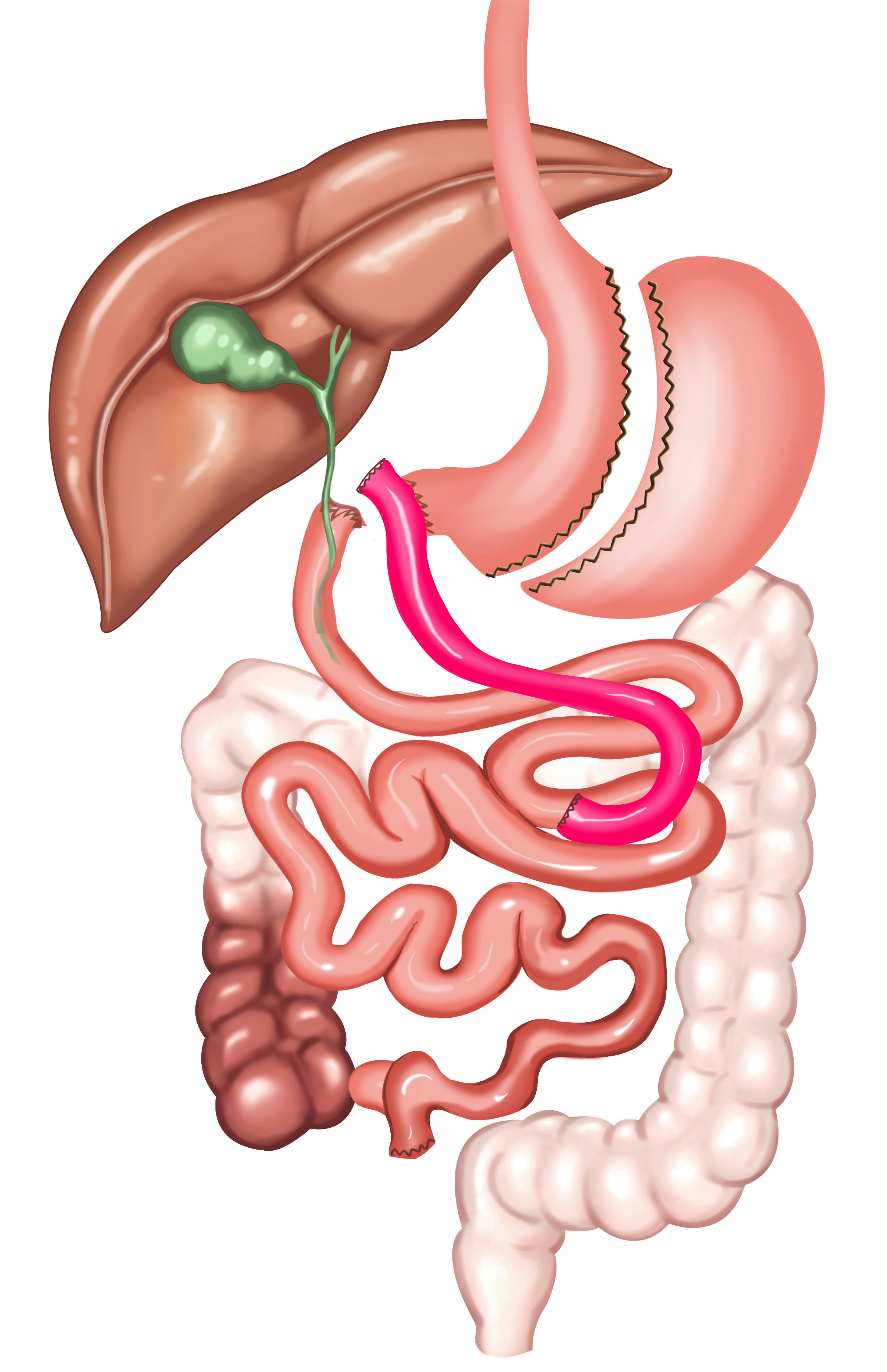 iii. Duodeno-Ileal Anastomosis
iii. Duodeno-Ileal Anastomosis
Ileal Interposition
iv. Ileo-Jejunal Anastomosis
Finally, lower end of ileal segment is connected into initiation of small intestine and the surgery is completed. So, small intestine of the patient is transferred to up. After Ileal Interposition surgery, absorption of foods from small intestines continue to be at highest level. No absorption defect appears. Our patients easily absorb vitamins and minerals from everything eaten.
Ileal Interposition and Hormonal Changes
Ileal Interposition operation functions as an endocrine surgery. Each procedure performed has a hormonal target and this hormonal change obtaines increases insulin efficiency.
Hormones Suppressing Insulin Effects
Hormones suppressing insulin effects are generally called as Anti-Insulinar System. The important components of this system include Glucagon, Resistin, Ghrelin, Cortisone, Adrenalin and Nor-Adrenalin. These hormones have periodical or permanent effects against insulin. Levels of these hormones are analyzed before the surgery and surgery is planned.
Glucagon: It is secreted from alpha cells of pancreas. It is secreted from cells adjacent to insulin secreting beta cells. It functions in opposite with insulin. It tries to increase blood glucose level. It increases glucose production in the liver. It reduces glucose use in the fat tissue and muscle. It is primarily responsible from insulin resistance occurred in the liver and muscle tissue. Glucagon levels decrease after the surgery or precautions are taken to reduce the efficiency even glucagon does not decrease. Stimulation of glucagon hormone to increase glucose production is eliminated by Ileal Interposition surgery. Furthermore, Insulin Resistance triggered by Glucagon disappears after Ileal Interposition. These effects present themselves on muscle tissue and fat tissue.
Resistin: Resistin hormone is another hormone causing insulin resistance. Resistin levels especially increase by intraabdominal lipoidosis. The site where interior organ lipoidosis occurs is liver. Liver is exposed to this lipoidosis from onset of Type 2 diabetes. When hepatic lipoidosis increases, fat deposits start to exist around other intraabdominal organs and especially on posterior side of peritoneum wall (retroperitoneal area). Resistin is secreted from this abnormal fat tissues and primarily responsible from insulin resistance on the fat tissue in particular.
Patients get rid of this abnormal intraabdominal organ and tissue lipoidosis in general after Ileal Interposition operation. By clearance of these abnormal fat deposits, Resistin levels regress to normal levels.
Resistin levels have a great important in assessment of metabolic weight of patients with Type 2 Diabetes. Resistin hormone that we detect higher than normal almost in all patients whom we plan obesity surgery because of morbid obesity is generally detected normal in slim patients. However, the case is not always same in patients with Type 2 Diabetes. Sometimes high Resistin levels may be detected in diabetic patients who are slightly over weighted as much as a morbid obese patent. These high Resistin levels are very important in these patients. Because, it is a better indicator for intraabdominal lipoidosis than abdominal circumference.
Even though resistin hormone is same in a fat patient and in a slim patients, metabolic problems of slim patient is severer than fat patient. This condition is that intraabdominal lipoidosis of fat patients is generally dependent to body fatness. Intraabdominal lipoidosis of slim patients are strongly and directly related with metabolic syndrome.
After Ileal Interposition operation, strong recovery obtained from resistin levels causes strong recovery pf metabolic syndrome findings as well. After Ileal Interposition surgery, 95% of our patients discontinue all cholesterol and hypertension drugs.
Ghrelin: Ghrelin is the main hormone which provides appearance of sense of hunger. The actual production region is fundus which exists on upper side of the stomach. Less hormone is produced from “E” cells in pancreas. The purpose to make gastric tubing (sleeve gastrectomy) by removing fundus part of the stomach in Ileal Interposition is to suppress secretion of Ghrelin hormone. Rapid reduction appears in Ghrelin hormone levels after Ileal Interposition surgery. Another cause for long term fullness sense that patients experience after the operation is reduction of Ghrelin.
Hormones Increasing Insulin Effects
Many different hormones or hormone-like substances are secreted from small intestines. These substances are called “incretin” or “secretin”.
 English
English Turkish
Turkish

